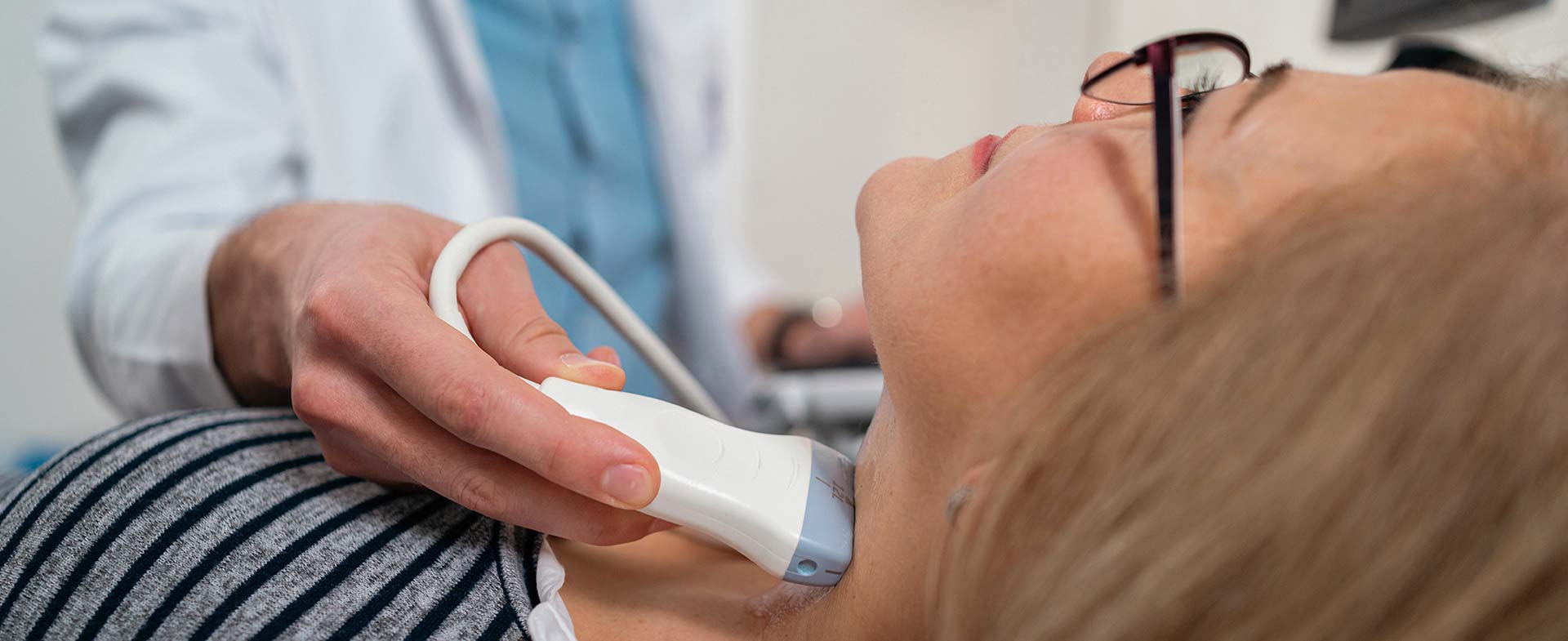
If you’ve felt your pulse at the side of your neck, you’ve detected one of your carotid arteries at work. The carotid arteries are two large blood vessels that serve as the main supply of life-sustaining blood for the brain.
But what happens when these important arteries stop working efficiently? Tamer Boules, M.D., a vascular surgeon with the Henry Ford Health, provides an overview of carotid artery disease.
What To Know (And Do) About Carotid Artery Disease
Carotid artery disease (or carotid artery stenosis) occurs when the carotid arteries become narrow or blocked. How does this happen, who’s at risk and what can you do? Dr. Boules explains.
“The carotid arteries become narrow or blocked with an accumulation of plaque,” states Dr. Boules. Unlike the plaque on your teeth and gums, the plaque in your arteries is a buildup of cholesterol, calcium, fibrous tissue and inflammatory cells. As plaque develops in the carotid arteries, less oxygen-rich blood flows to the brain. More commonly, it is possible for a piece of plaque to break off, travel to a smaller artery in the brain and block the artery - suddenly decreasing blood flow to that part of the brain.
Carotid Artery Disease And Your Risk For Stroke
The greatest risk of carotid artery disease is stroke, especially as the blockage becomes more advanced. Yet, not all people who have carotid artery disease will have a stroke. “Blockages in the carotid arteries can decrease blood flow to the brain and cause a stroke,” Dr. Boules explains. “But it’s not a given. In fact, strokes can often be prevented with the right medical care and by taking charge of your health.”
“Some people with carotid artery disease don’t have symptoms until they have a stroke or transient ischemic attack (TIA)," notes Dr. Boules. Symptoms of stroke and TIA include:
- Difficulty speaking
- Facial droop
- Losing feeling and function in your arm, leg or face, often on one side of your body
- Sudden loss of vision
“Transient ischemic attacks, which have symptoms that subside in less than 24 hours or even a few minutes, are not minor events,” cautions Dr. Boules. “They can lead to major ones. Despite being painless, all stroke symptoms require immediate medical attention, even if the symptoms disappear soon after. The sooner treatment is initiated, the lower the risk of permanent brain damage."

Vascular Care At Henry Ford
Treating Carotid Artery Disease
“Patients often think carotid artery disease means surgery, and that surgery means a long recovery,” remarks Dr. Boules. “But there are new techniques and treatments to manage carotid artery disease.” Treatment options include medication, such as daily aspirin and cholesterol-reducing and plaque-inflammation-reducing medicines, as well as surgery and lifestyle adjustments.
“If surgery is the best option, it may involve removing the plaque during an operation or implanting a stent into the artery. With those procedures, most people go home the next day and are back to work within a week.”
Taking Charge Of Your Risk Factors
Who is at risk for carotid artery disease? “If you smoke, are overweight or have high blood pressure, diabetes or family history, you could be at risk for carotid artery disease,” advises Dr. Boules. “If you have multiple risk factors or have had a stroke or TIA, talk with your provider. Diagnosis typically includes imaging, such as ultrasound or a CT scan.”
Your vascular surgeon may work with your primary care provider as well as other experts from cardiology and neurology to make sure they are finding the treatment program that is best for your and your long-term health.
“You can improve your health through education and lifestyle changes,” says Dr. Boules. “Understand your family history and risk factors to make healthy changes. Stop smoking, control your blood pressure, follow a heart-healthy diet and get daily exercise.”
Dr. Boules emphasizes the importance of following your doctor’s orders. “If you’re taking medications, such as aspirin or statins to prevent stroke, follow your provider’s instructions. Do not stop taking a prescribed medication without discussing with your doctor first. Medication can help stabilize plaque, stop progression of the disease, decrease the risk of death and more.”
Reviewed by Dr. Tamer Boules, a vascular surgeon who sees patients at Henry Ford West Bloomfield Hospital.